By: Dr. Ehud Sasson
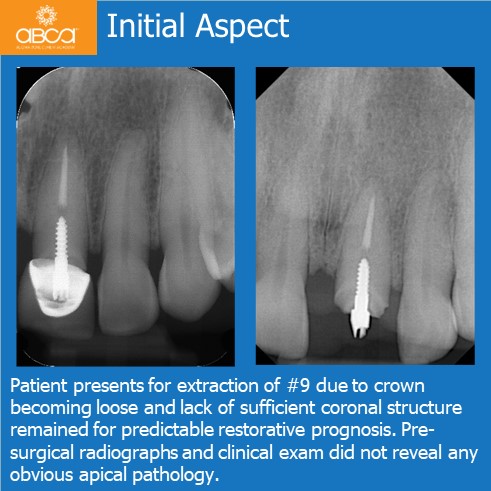
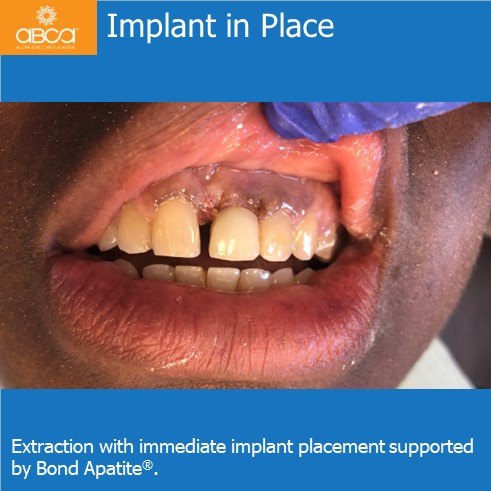
The patient presented for extraction of tooth upper left incisor due to a lose crown. There is a lack of sufficient coronal structure remaining for a predictable restorative prognosis. Pre-surgical radiographs and clinical exam did not reveal any obvious apical pathology.
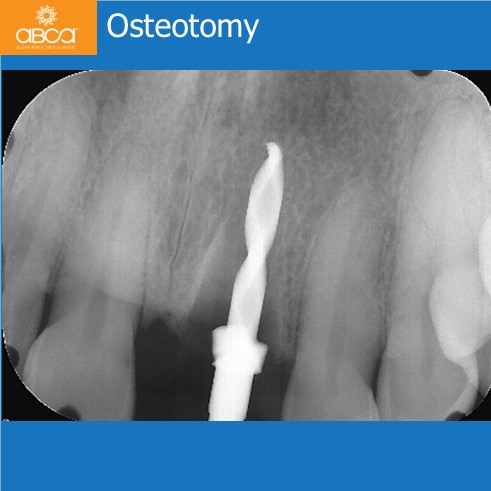
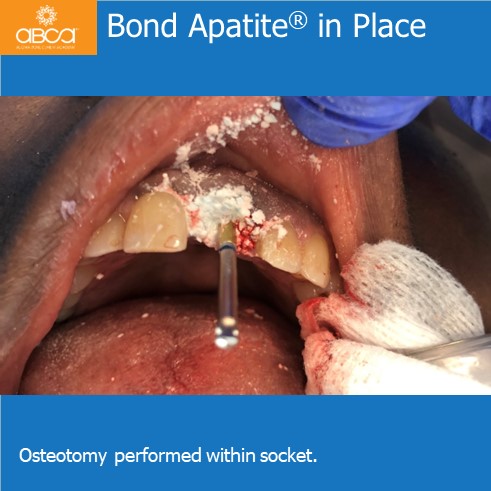
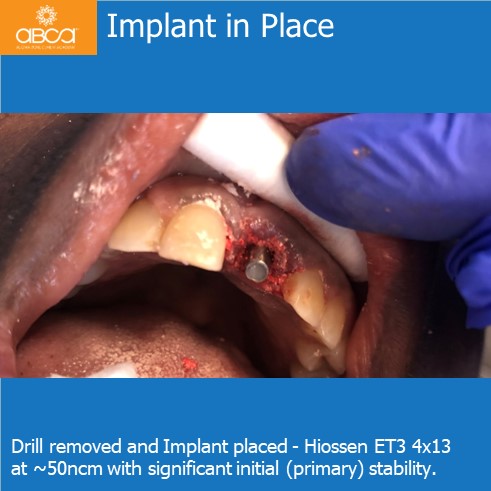
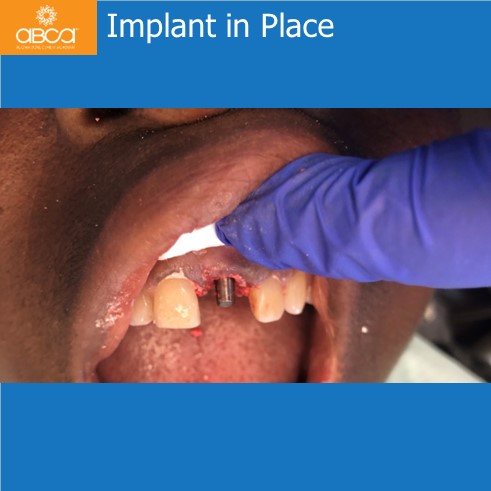
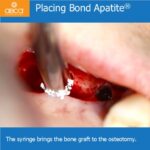
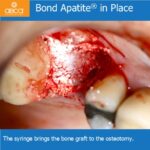
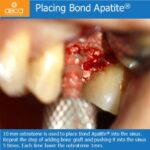
Surgery was performed with a full thickness flap and the tooth is extracted atraumatically and intact. Osteotomy was performed within the socket. While the final drill was in place of the osteotomy, 1 cc of Bond Apatite® was placed around the drill and overfilled in the socket. The drill is removed and the implant is placed with significant initial (primary) stability.
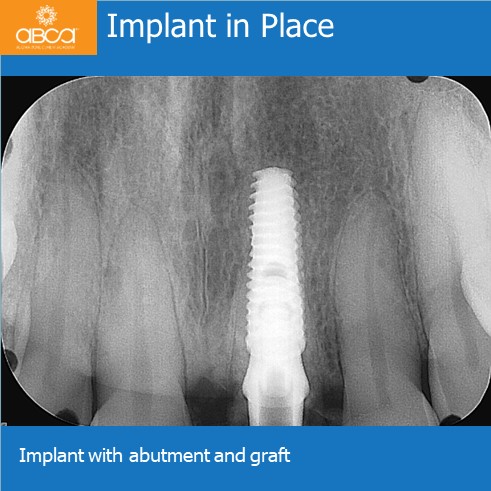
A prefabricated abutment was inserted, adjusted for proper contour, and only hand tightened at this time. Using a stent a Bisacryl temporary crown was fabricated initially intra-orally. Composite added to the crown and then cemented to the abutment while extra-oral. An abutment with a crown was inserted and torqued to 25ncm. The screw access hole was closed with cotton and composite.
A collagen dressing was placed above the Bond Apatite®. Chromic gut sutures used mesially and distally, not overly tight with the intent to keep shape of original soft tissue intact. Occlusion was adjusted and post operative instructions given with emphasis on avoiding occlusion on the temporary crown.
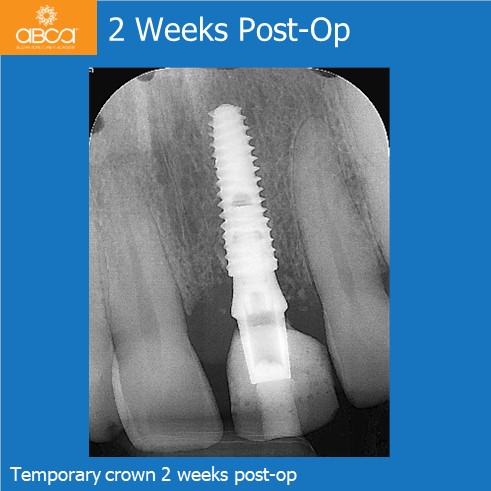
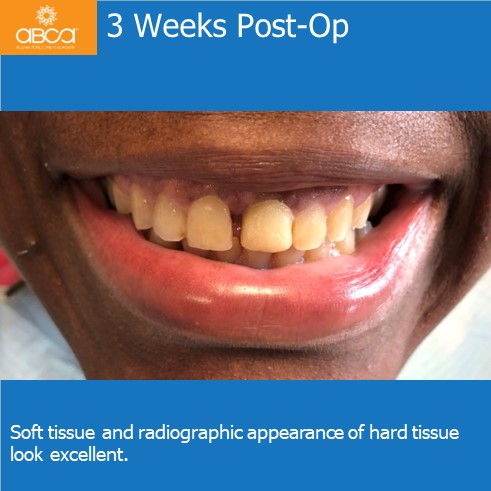
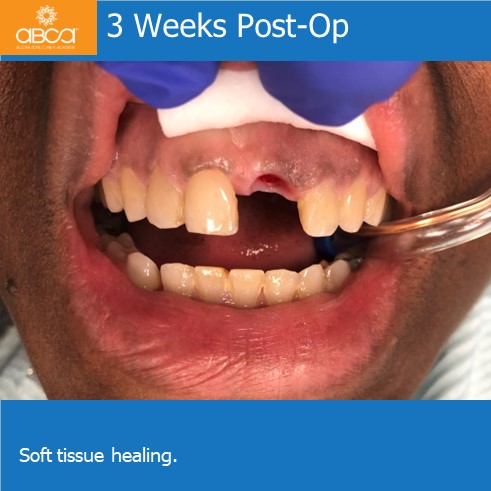
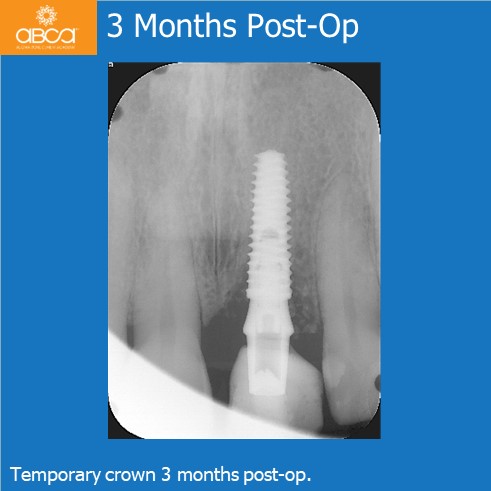
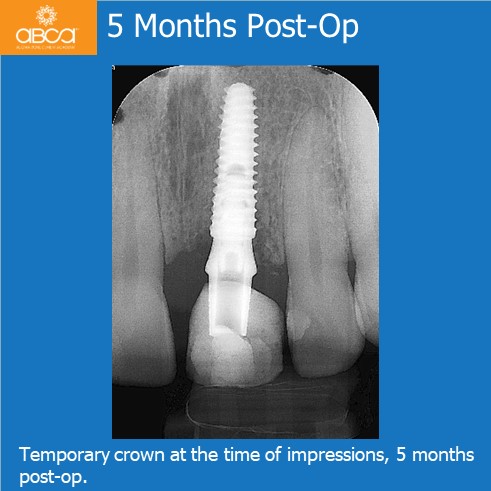
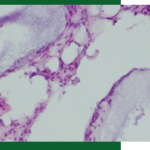
At the 3 week follow up soft tissue healing was excellent, and the radiographic appearance of hard tissue looks excellent. Two months later the crown became loose and was re-torqued with a temporary abutment/crown. 20 weeks post-op impression were taken for a final abutments and crown. Soft tissue looks excellent.
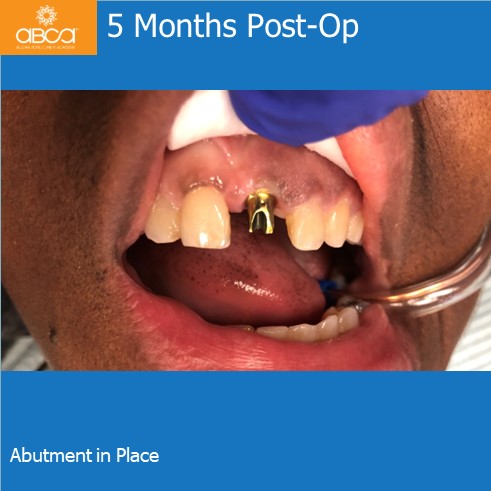
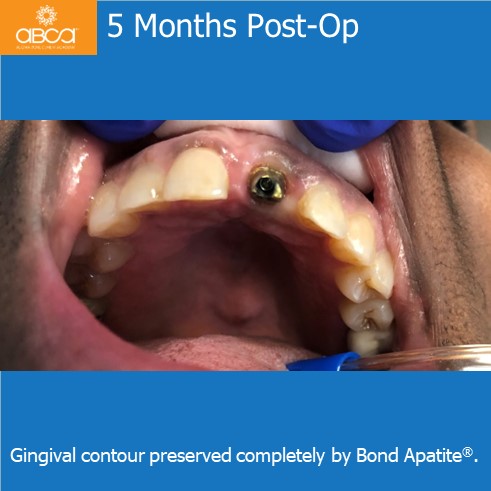
5 months post-op the final abutments is inserted. A temporary crown is placed at this time and the final crown is sent back to the lab for custom stain.
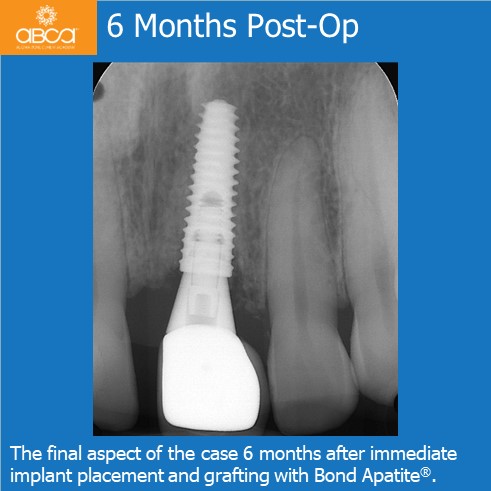
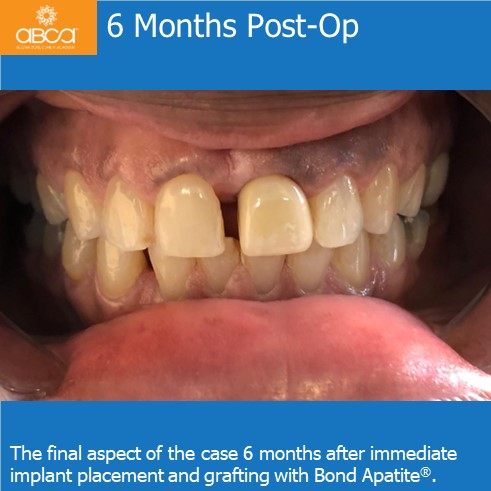
6 months post-op final insertion of the permanent zirconia with layered porcelain crown is placed.
“Screw-mentation” technique = Cemented intraorally and then removed abutment/crown via screw hole access to ensure cement removal.
Occlusion adjusted.