Augma’s revolutionary materials open a whole new world of opportunities. Biphasic Calcium Sulfate enables us to perform protocols which are less invasive surgical procedures with full tension on the flap without using a membrane, all while maximal closure is sufficient – the only material in the world to allow this. Thus, giving the graft maximum stability, the least invasive procedure for the patient, and for you, the clinician, the ability to predict a successful outcome from day one! To enjoy the benefits of Augma bone graft cement we must respect these guidelines and understand why it’s crucial to follow them.
Why Full Tension Flap
Why with biphasic calcium sulfate bone cement the flap should be with tension and not tension free as with conventional bone grafting procedures?
With conventional bone grafting, tension free flap and primary closure are mandatory. Otherwise, the graft will get exposed, and we might end up with contamination and graft failure. The reason for that is because biologically soft tissue healing starts by retraction. Due to the fact that the interaction between the soft tissue and graft or membrane underneath doesn’t allow normal healing by proliferation, the flap will continue to retract, and the graft will get exposed. Thus, to compensate for this retraction, the surgical flap needs to be tension free.
The problem with tension-free surgical flap is that the soft tissue manipulation is more invasive, larger flaps are needed to expose the host site, and dissection of the flap compromises the blood supply, and the flap becomes connected to the muscles’ movement, and so it requires higher surgical skills, and it is more traumatic to our patient, (swelling, pain, hematomas).
In contrary, calcium sulfate has impeccable synergy with soft tissue, and the ability to enable the quick and safe proliferation of the soft tissue over its surface without any risk of contamination during exposure due to the graft bacteriostatic nature. The stable structure of the biphasic calcium sulfate cement keeps that proliferation above the surface more predictably.
These characteristics of biphasic calcium sulfate enable our patients to benefit from less invasive surgical procedures; the procedure is fast and less complicated, and no involvement or influence of the muscles on the flap stability (the flap and the graft is kept stable during the healing phase). As a result of minimal flap reflection and lack of muscle involvement with the flap, post-operative pain is minimized, hematomas are practically not apparent, and swelling is significantly reduced.
There is no need for higher soft tissue manipulation skills and experience while applying the graft material, and it is extremely easy for us as clinicians.
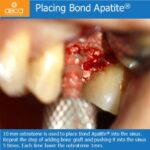
All is needed is to reflect the flap only 3 mm beyond the MGJ to place the cement and stretch the soft tissue for closure (3 mm into the mobile mucosa will enable 6 mm stretching together with 3 mm of graft exposure we can have a potential 9 mm of horizontal width) which is sufficient for almost any horizontal volume loss.
It is a huge advantage for our patients and us. Something that we didn’t have up until now.
Why No Membranes
Why no membranes or PRF or any additives should be placed between the cement and the flap?
Unlike common graft materials, which require containment, BCS cement does not need that.
In fact, even for allograft or xenografts or other particulate alloplasts, membranes are not needed for the graft to convert to the bone. The reason, however, membranes are a MUST with those products is due to containment. Without containment, the particulate grafts will migrate everywhere under the loose flap (since the require tension-free primary closure) and the graft will fail on volume and quality (the result will not be bone since there will not be particulate cohesiveness).
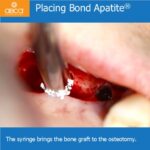
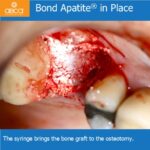
This fact makes all the difference. The BCS is self-contained. Once placed and pressed in to place as described by our protocols, the graft stays there and closure of the flap should proceed right away.
A membrane or any intermediary between the cement and the periosteum is a disadvantage here since it will require a tension free flap and primary closure (more invasive as well as graft stability will be jeopardized by muscles’ movements) and healing will be delayed due to the blocked periosteum which has high osteoprogenerativity value. Unlike other graft materials, the BCS cement is bioactive. Its osteogenesis and angiogenesis capabilities are activated throughout the graft volume. As the graft resorbs, simultaneously the bone formation takes place. Thus, having a membrane containment over the graft will actually impede this unique bioactivity of the cement. For best results, a continuous cohesive crystalline cement matrix is the goal. That matrix HAS to be in direct contact (flap closure with tension) with the host tissue from all directions to achieve maximal regenerative potential.
Why Maximal Closure
How come maximal closure (3 mm of graft exposure) is acceptable and primary closure is not mandatory?
In our institutional (substitute “old”, or “classic” if one wants to feel better) surgical training, primary closure is the gold standard for a successful graft procedure. The reason for this is the fact that most graft materials are prone to bacterial contamination and infection. This complication will result in total graft loss and increased surgical morbidity for the patient. Most graft materials are particulate and unstable and thus require a containment device (mesh, membranes etc.) which are also prone to infection if exposed or tend to compromise blood supply to the healing host site. In fact, some of these containment elements (Teflon membranes, ti-mesh, ti-reinforced membranes etc.) by their nature, can cause the exposure of the graft. Thus, primary closure is non-negotiable in these situations.
BCS Bone graft cements offer a paradigm shift. The nature of the cement being its ability to adhere to the host site and harden is situ negates the need for containment devices in most augmented clinical cases, thus various membranes or meshes are not needed. The chemical salt structure has bacteriostatic abilities, and the bioactivity of the BCS cement generates a high calcium ion concentration enhancing bone formation and rapid soft tissue proliferation above the graft surface with minimal risk of contamination during exposure. Thus exposure of the graft material is irrelevant from the aspect of bacterial contamination. Due to these facts, primary closure is not necessary.
When the cement sets and if properly handled, as directed by our protocols, a continuous crystalline matrix is initially formed. This matrix (the set cement) is actually conducive for soft tissue propagation. Thus, even if exposed, the cement will allow the soft tissue to proliferate over its external surface, to achieve closure by secondary intention. Leaving an incision open more then 3mm will result in volume loss, since the cement dissolves, as part of its conversion to the bone, and too much of an opening will allow the material to escape.
Thus, the real reason we recommend maximal closure (if primary is impossible) is to protect the patient and the wound site. To allow you, the clinician, to efficiently and expeditiously conclude the procedure without unnecessary and irrelevant surgical aggression.