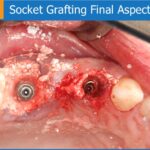
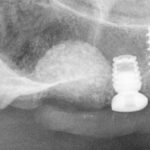
The patient is a 52-year-old healthy woman. She presents with a failing 3-tooth bridge with movement, infection and bone absorption of tooth #16 (3). The patient complains of pain when…
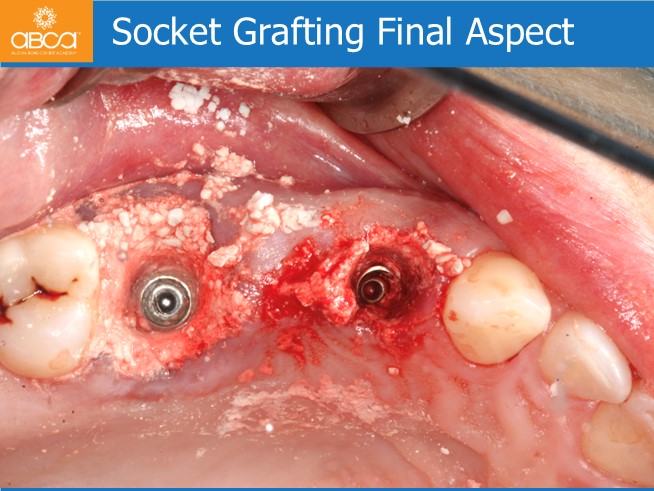
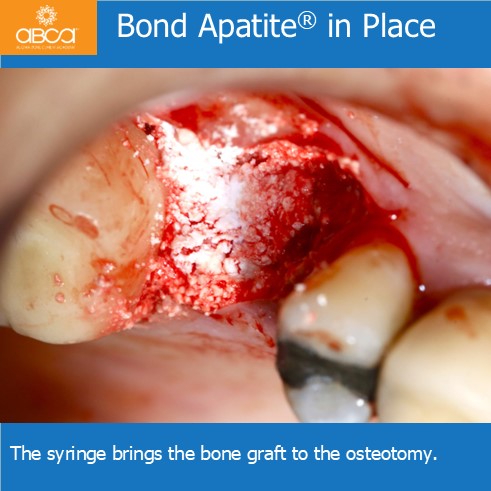
Sinus lift with Augma Lift™ Kit B when there is 6 mm Sub Sinus Bone Height
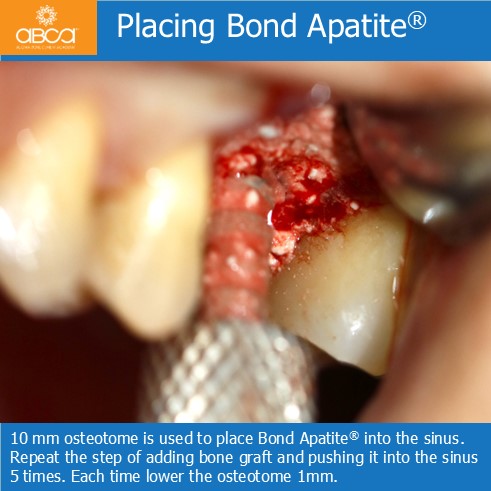
Sinus lift with Augma Lift™ Kit B when there is 6-7 mm Sub Sinus Bone Height.
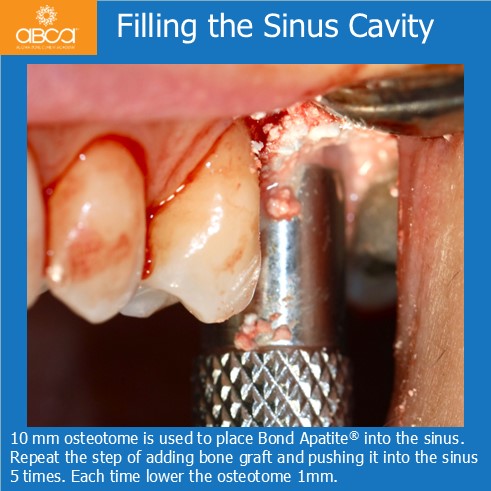
Sinus lift with Augma Lift™ Kit B with 4-5 mm sub sinus bone height. A young woman came to replace the missing first maxillary molar with moderate atrophy.
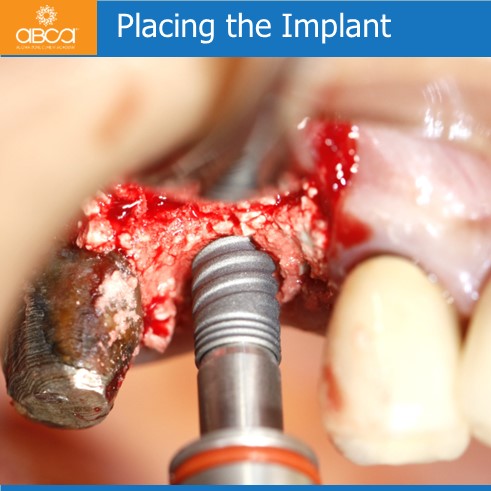
Sinus lift with Augma Lift™ Kit B in a case with 5 mm sub sinus bone height.
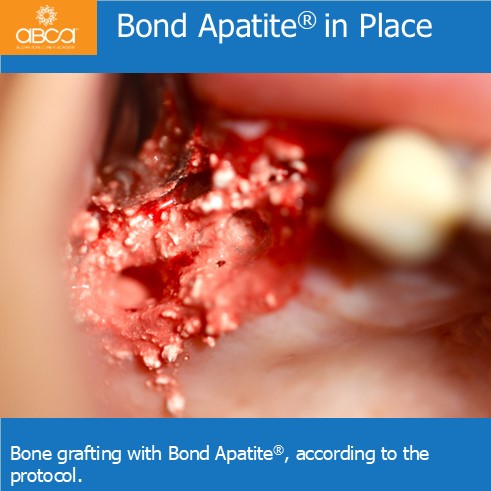
Sinus lift with Augma Lift™ Kit B in a case with 5 mm sub sinus bone height. The patient came for implant treatment in the region of teeth #16 (3)…
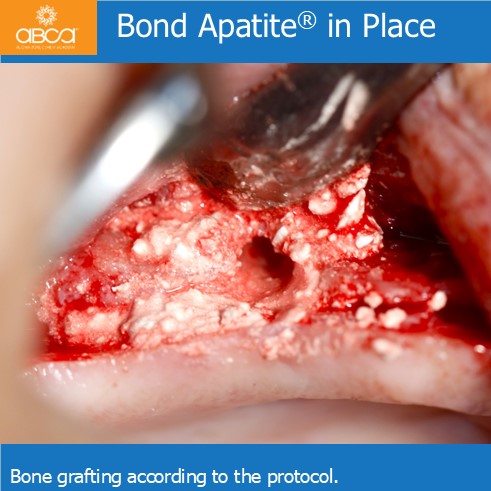
Sinus lift with Augma Lift™ Kit B in a case with missing teeth #14 (5), #15 (4), #16 (3), #17 (2) and a sub sinus bone height of 6 mm.
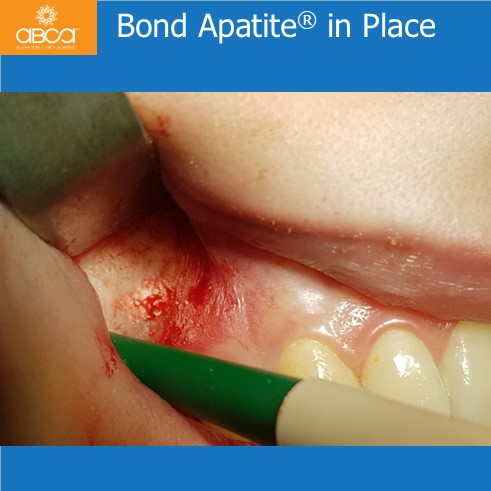
The patient is a healthy, 23-year-old female. The small cyst was discovered after she had a little pain in area of tooth #15 (4). Tooth #15 (4) was treated endodontically…
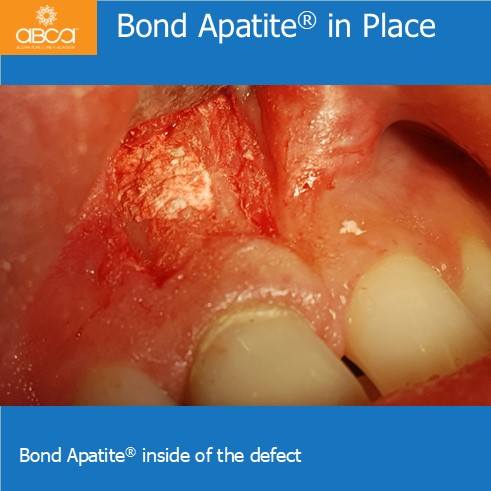
The patient is a healthy, 20-year-old male. The small cyst was discovered after experiencing strong pain in the area of tooth #11 (8). Tooth #11 (8) was endodontically treated twice.…
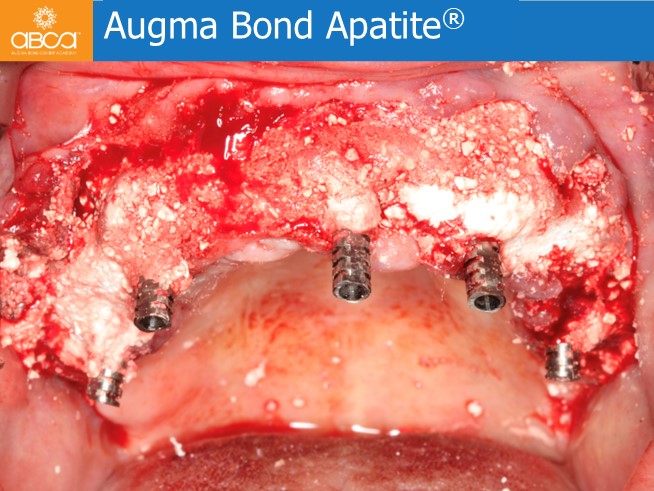
The patient is a healthy, 63-year-old female, who attended the consultation complaining about a lack of aesthetics of her smile and difficulties in chewing properly. She had a failing, old…